Dr. Ruby Wang is a practising UK-trained doctor with over a decade of experience across clinical medicine, health policy and health technology. Born in China, she moved to the UK at a young age, and her subsequent career has focused on bridging the East and West, starting with studying as a Schwarzman Scholar at Tsinghua University. She has gone on to work as a medical adviser at Alibaba Group’s AliHealth, a health advisor for the United Nations in China, and served as the head of Health at the British Embassy in China. There, she led the UK Government’s health diplomacy in China, including negotiating with China’s major healthcare bodies. She is the founder and managing director of LINTRIS Health, an award-winning consultancy that bridges health and life sciences across East and West. Dr Wang regularly speaks and writes about the intersection of innovation and global health with a focus on China. This includes her ChinaHealthPulse newsletter, where she spotlights key trends in global health, policy, and technology. She is currently writing a book on China’s health innovation.

Illustration by Lauren Crow
Q: To start with, can you briefly explain how the Chinese health system currently operates?
A: China’s health system is quite distinctive. It blends the requirements of a massive population and the huge burden that demands in terms of disease volume and patient needs, with the unique governance and centralized policy making of China’s particular political structure. Unlike the UK’s National Health Service, Canada’s single-payer system, or the U.S.’s more capitalist-driven health care system, China’s health care really operates as a patchwork of public and private actors.
There are two main pathways to healthcare. There is a high volume of universal health coverage from a reimbursed public system, with huge hospitals that handle massive patient volumes affordably. So most people can access some form of universal health coverage via the national health insurance system. There’s a lot of disparity depending on where you are, if you’re in a rural region versus an urban city, and even between cities; and there’s a lot of variation based on the quality of service you might get. But overall, there is a baseline level of insurance that is partially or fully reimbursable.
| BIO AT A GLANCE | |
|---|---|
| AGE | 33 |
| BIRTHPLACE | Hangzhou, Zhejiang, China |
| BASED IN | London, UK |
Alongside that, there’s also a growing private sector that can offer faster and more comfortable — albeit higher-priced — services for which consumers pay out of pocket.
Both of those work in parallel. If you’re a patient, depending on if you’re in a city or in a rural setting, and depending on what you can afford or what you can access, you can move between both the public and private systems at will, sometimes even within the same episode of care. It’s a lot more flexible than the U.S. or the UK. But it also makes the system more complex to navigate, especially for outsiders wanting to understand it and make the most of it. If you’re an investor or in pharma it is quite hard to know how to operate within that system.
| BIO AT A GLANCE | |
|---|---|
| FORMER POSITION | Head of Health for the UK Foreign Office in China, Health Advisor for the United Nations Resident Coordinator in China, Medical Advisor at AliHealth, Alibaba |
| CURRENT POSITION | Practicing UK doctor, Director at LINTRIS Health (a consultancy bridging east and west in health policy, biopharma, and medtech), founder of the ChinaHealthPulse newsletter, and Digital Health Council at the UK Royal Society of Medicine. |
For a patient in China’s healthcare system, what would a typical experience be like?
As an example, when my grandmother goes to the hospital with some foot pain, she can go on to WeChat, find the mini app [for the hospital], click on it, and scroll to the doctor she wants. She can probably find a time slot for the same day, and book it. Then she can book herself a DiDi [taxi] to go to the hospital, walk in, and won’t really have to wait because her appointment message has told her which part of the hospital to go to. She sees the doctor: They maybe only have five minutes, but they’ll sort out whatever she needs. She can maybe book a blood test, a scan, or an x-ray. She can do that all on the same day in the hospital.
If the doctor prescribes medication, she takes that down to the prescription floor, pays via her phone, and gets the medication. For the insurance reimbursement there’ll be a counter in the hospital, or she can process that through her phone. She’ll typically get all the money back for the visit. Every person will have some form of universal health insurance, and they will at least get a sizable portion of the costs back.
Tech is built into daily life now in China… In health, it’s moved from pilot projects to institutionalized infrastructure. It’s becoming, not to be dramatic, the backbone of the Chinese system, ensuring that care can be accessed at scale.
But there’s a limit for that basic healthcare. There’s still a lot of disparity, because it’s a huge country from an economic and social point of view. You still have really remote regions where people don’t have access to basic daily life needs, and healthcare is included in that. In cities like Shanghai and Beijing, there’s a different tier of health services.
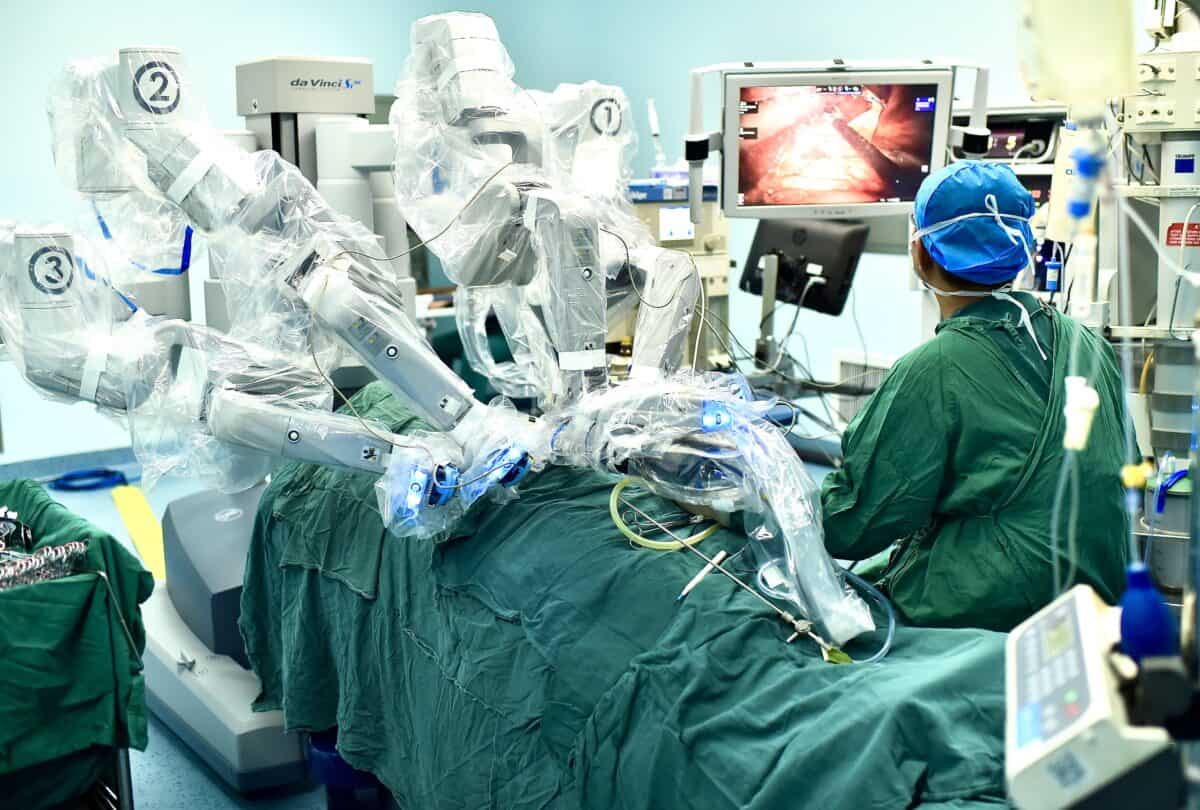
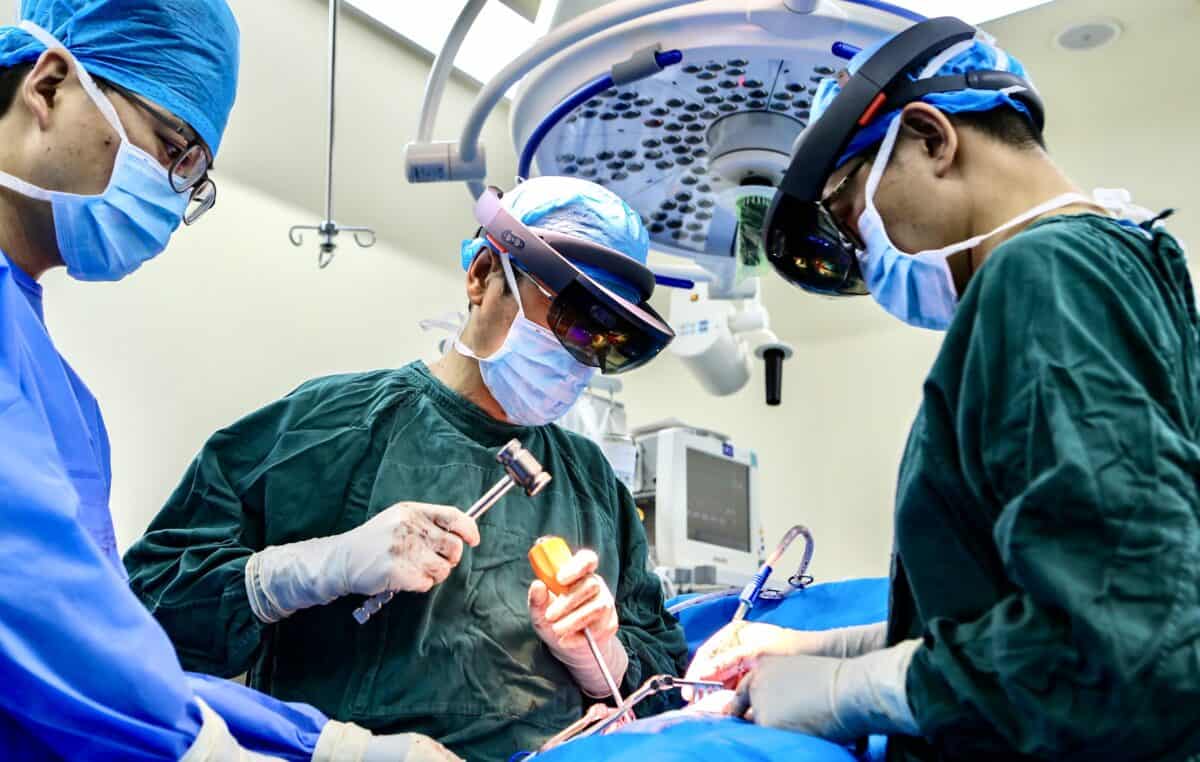
Left: A surgical robot performs a cardiac surgery, Anhui Medical University Hospital. Right: Doctors use Mixed Reality headsets during a spinal correction surgery, Xi’an Jiaotong University Hospital. Credit: Depositphotos
Cancer is a very difficult area, because depending on the specific type of cancer and the drugs available, some treatments aren’t covered by the basic insurance.

In terms of insurance, China has a unique system based on what’s called the National Reimbursement Drug List (NRDL). When it first came into play in 2018, everyone was trying to figure out what it was, especially the foreign pharma companies. Essentially, it is a list of drugs which can be reimbursed through basic insurance, guaranteeing people access to key medications. The Chinese government negotiates the prices of these drugs and buys them in volume, making procurement more affordable. Depending on the drug, it can cut the price by up to 90 percent. The whole idea is volume-based procurement: Even if a pharma company sells a particular drug at a very much reduced price, if the volume sold is still in the millions, then it will still be making enough revenue from it.
Alongside this strong public health system, China is increasingly looking to boost its private health, as it faces the health burden of a large and aging population. New foreign private hospital licenses are being issued, and a commercial drug insurance list has been expanded nationwide, making higher-end drugs beyond those available on the NRDL accessible on private health insurance. There has even been policy support for medical tourism. This increasing privatisation of China’s health system will have significant implications for patients, providers and industry stakeholders operating in China.

A lot of people will understand China’s healthcare system based on what they read, or even maybe experienced during Covid times. How different is the system today than the system that existed before then?
The main thing Covid enabled was an acceleration of digitalization. We’ve seen it in the UK and in the U.S. as we were forced online, but in China, the digital transformation of healthcare was already in process. Covid has just meant that it has become a permanent part of the healthcare infrastructure.
Supporting this is a very different view of privacy. China’s population, culturally, is less wary of data privacy. They’re more willing to share their data for convenience. The Chinese government is also very keen on digital, AI, and data governance. Even pre-Covid, social platforms like WeChat and Alipay were already prevalent, so scanning QR codes for payment was normal.
Health was always a sector that was going to have a slower digital transformation due to regulation, and safety and ethics concerns. However, Covid catalyzed the transformation. In 2019, I did a project on internet hospitals. At that time, there were 350-400 internet hospitals in China. The last measured count in 2023 was 3,000. Today, all brick and mortar health services must have a digital service: If you don’t, no one will come to you. An internet hospital is a licensed healthcare provider which combines three main pieces: online consultation, online pharmacy and online payment. If you loop those three pieces together, then you’ve got an imperfect pathway, but still a pathway, for health service provision.
Tech innovation is a really big part of healthcare. What are some of the innovations you are seeing in China?
Tech is built into daily life now in China, in messaging, food delivery, payments and now access to health care. It’s expected by the population, and it’s been tested and accepted with confidence by the government. It’s just part of life now, seamless and embedded into the way people live day to day.
In health, it’s moved from pilot projects to institutionalized infrastructure. It’s becoming, not to be dramatic, the backbone of the Chinese system, ensuring that care can be accessed at scale. This is really important, because we’ve never seen this done before in other countries. China historically had a lot of respect for and wanted to learn from the UK model, where primary care is key. In Britain, GP practices [GPs, or general practitioners, are local doctors who are the first contact for most patients in local communities in the British system] provide a gate-keeping mechanism to ensure accessibility and cost and efficiency, because tertiary, specialist care is more expensive. However, now with technology, you don’t even need anything like a GP practitioner; you can just use an online platform to access tertiary care.

China is now already implementing this model in the Global South. It’s teaching those lessons to other developing countries who also don’t have the luxury of building traditional bricks and mortar health infrastructure, or hospitals at scale or at cost. Digital is really paving the way for greater accessibility, affordability, quality of care, and equality. Those are the four pillars of healthcare, so tech is really exciting for health in China.
With the massive disease burden and shortages of clinical professionals in China, there was a fast uptake of technology in healthcare. There’s real pressure and a real appetite for integration of tech into health. An example is that following various fake drugs and illegal drugs scandals, China’s National Healthcare Security Administration began piloting a big data platform in 2024 which created a code for every package of drugs sold. This allows for the tracing of who prescribed the drugs and who they were prescribed for. You can’t sell the drugs on, and you can’t give them to the wrong person.

Now, this system has expanded from a few provinces to become nationwide. Nearly every single prescription box of drugs in China is labeled and coded so that it can be fully tracked, an incredible feat for a country this big. That speed and that scale is unmatched across any other country in the world, and that is just one example of how quickly China moves, even in a sector like health.
If we talk about AI, I don’t think anyone who works in health AI in China thinks about it as a separate concept anymore. They just expect some kind of complex large language model or machine learning mechanism to make sure that tech is enabled in healthcare. Whether that’s surgical robotics or diagnostics and therapeutics, AI tools can assist.
Even with AI and internet hospitals, there are shortages of trained personnel. Young doctors often have to involuntarily rotate out for mandatory service in remote regions. So rural-urban gaps persist despite technology coming in to plug those gaps.
One very good example is Alibaba’s DAMO (Discovery, Adventure, Momentum and Outlook) Academy, a global research institute founded by Alibaba in 2017 with a vision to use technology to advance humanity. I’ve heard Jeff Zhang, its head, talk about how he believes health is the first and most important sector that AI will change. They have been doing a lot of work into AI imaging and diagnostics.
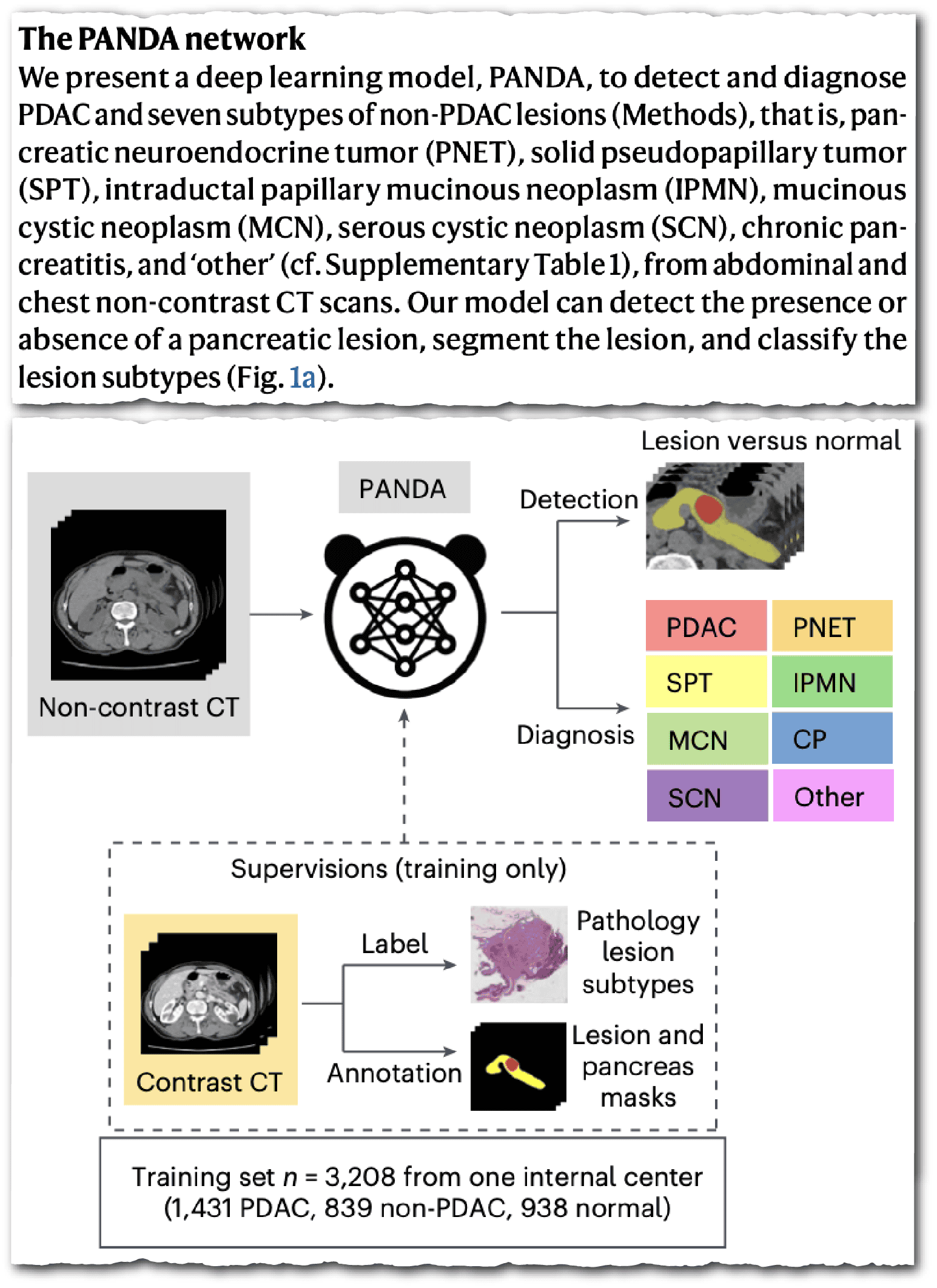
They recently came out with PANDA (Pancreatic Cancer Detection with Artificial Intelligence), which is a method for diagnosing early-stage pancreatic cancer using artificial intelligence. For me, as a clinician, it blew my mind. Throughout the whole of medical school we were told statistically that pancreatic cancer is one of the deadliest cancers. By the time you diagnose it, it’s usually spread to your liver, causing jaundice, and it’s too late. There are very few treatments and usually 90 percent of patients pass away within a year of diagnosis. However, this PANDA AI tool can diagnose pancreatic cancer at the early stage. It’s now been approved by the U.S.’s Food & Drug Administration. It’s not been talked about much in the wider media, but for the scientific clinical community, it’s groundbreaking.
Moving away from technology, there’s been lots of talk about a so-called ‘silver economy’, shifting the focus away from China’s aging population as a risk to being an opportunity. But what is China’s health care system doing to try and deal with the country’s aging population?
It’s a really interesting question, a challenge that’s shared by Japan, the U.S., UK and now China. The aging population is a huge issue for two reasons: Older people are becoming a greater health burden on the state and the economy, but at the same time, it means the healthy workforce is reducing.
China is doing various things on an experimental basis. We see media releases about a ‘silver’ carriage on a high-speed train with handles and doctors on board, or first aid kits to support tourism for the elderly population. When I went back to Beijing recently, I saw community gyms in Ritan Park, and a lot of elderly people were working out. Having these fully digitized, free gyms is really nice. So, they’re injecting a lot of capital: however, it’s unequal. The way it’s been rolled out is experimental: depending on the regional resources, and if they succeed or not based on localized uptake, they will keep going.
With healthy aging it really depends on the consumer uptake. The traditional Chinese family model is that the elderly are looked after by the young. However, the legacy of the one child policy means there are often four grandparents to one grandchild, so that’s not really possible. Asking Chinese friends how their grandparents feel about this, there’s diverse opinions. In the cities, I’ve had friends explain their grandparents are aware they will need to live in a care home. I was surprised, because I would have thought that would be culturally unacceptable. However, my friends’ grandparents were aware of the reality that the young simply can’t look after them.

However, in more rural settings, where there’s a more traditional mindset, there is still an expectation, especially if the grandparents have looked after the grandkids while the parents have been away. There are a lot of cultural and societal shifts in China in unexpected ways, and we’ll see that play out.

Overall, in terms of the silver economy narrative, China’s doing bits and then seeing what sticks. In terms of policy implementation, it’s still relatively early days. Despite the hype, lots of families still provide unpaid care, while palliative care is really under-skilled in China. Certainly from a governance point of view there’s an increasingly intentional strategy. What China always does is lay out high-level strategies, and then the officials at the local level will start implementing that strategy. In a few years time we’ll see the outcome, but I think we can be pretty confident in saying that whatever happens, China will be doing it with more intent and more quickly than we will see in the West.
You have talked a lot about the positives, but there are obviously still plenty of flaws and issues in China’s health system. What are areas that still need improvement?
Firstly, the uneven access to healthcare, especially with the rural-urban gap. Even with AI and internet hospitals, there are shortages of trained personnel. Young doctors often have to involuntarily rotate out for mandatory service in remote regions. So rural-urban gaps persist despite technology coming in to plug those gaps.

Secondly, the massive health burden persists. The hospital-centric system is still overwhelmed. Tertiary care, despite a push to community level and better tech helping, still has patients flooding specialist services for minor issues, especially in some medical specialties like mental health and geriatrics, where it is very difficult to hire specialists as the work is seen as low status or underpaid. There’s still a long way to go, with demand too high especially as people live longer.
Finally, data fragmentation is another issue. Even with high quality data integration, sometimes poor interoperability and uneven digital rollout across regions means hospitals still don’t use systems that talk to each other. China’s health coverage is very patchwork, it’s not geography based with one area managed by one organization. You have different hospital brands, public or private sector, all in the same area. You can log into the mini app and access your own blood test very quickly, but you can’t send that across to another hospital. I’ve heard this is an increasing focus from a policy point of view. We talked about the drug boxes, which was the easiest reform to implement; now blood tests are the next level that they’re working on to integrate into a national system. A unified digital ecosystem is still something for the future. However, I feel again that China is going to be setting the standard.

You recently returned from spending a significant amount of time on the ground in China. What have been some of your experiences there?
Every time I go to China, I visit hospitals to do my own field research. I can give you 10 anecdotes about going to hospitals that were incredible. High-end services, marble lobbies, shiny corridors, and all at the scale and size of airports — not just in major cities, but also increasingly in smaller towns. I visited my grandfather in Tonglu, a lower-tier city in Zhejiang Province. There was a brand new hospital, and it was the fanciest hospital I’ve ever set foot into in my life, even compared to Beijing and Shanghai. It was like stepping into Doha airport, everything was shiny and new, and the wards were fully digitized.
I also visited community clinics in cities that all had cloud-based systems. At every level there was evidence of tech-enabled platforms, even in the parks at those outdoor gyms.
I think it’s really important to be aware that China is so far ahead in health, and it’s a shame not to pay attention. What it does in health is going to impact patients, populations, and all levels of healthcare for every country.
However, I can also tell you that in Shanghai, I went into a hospital in person to try to book an appointment, and they wouldn’t let me. You could only book digitally, and because I had a foreign passport, they just couldn’t register me. Even though I was there in person, I couldn’t actually see a doctor.
| MISCELLANEA | |
|---|---|
| FAVORITE MUSIC | Hiphop or classical. |
| MOST ADMIRED | Elizabeth Garrett Anderson. A woman of many firsts! The first woman to qualify as a doctor in England, the first female founder and dean of a medical school, and later on the first female mayor in Britain. |
Finally, you’ve told us how China’s healthcare system has been evolving. What are the consequences of this for the world?
People tend to see healthcare as a very specialised sector, in the domain of scientists and doctors. Many don’t think of their own health until they become ill. Crises such as Covid show we must all be paying attention. Diseases have no borders, and we are all sharing the same challenges in healthcare.
I want to emphasise just how fast the tides are changing. Previously, we saw a lot of Western assets, such as new drugs, being co-licensed and sold inbound into China. But now we’re increasingly seeing Chinese-created assets being licensed for sale abroad. In previous years, Western best practices were being applied to China and Asia, but now it’s the other way around. Chinese biotechnology companies are really trying to get into Europe and the United States, while China is also applying digital healthcare models in the Global South. China’s not catching up, but innovating and looking outward with increasing confidence.
| MISCELLANEA | |
|---|---|
| FAVORITE BOOKS | I like thoughtful books with great prose, for example Wolf Hall by Hillary Mantel, and Anna Karenina by Leo Tolstoy. |
| FAVORITE FILMS | Fantastic Mr. Fox by Wes Anderson and Lord of the Rings, of course! |
I think it’s really important to be aware that China is so far ahead in health, and it’s a shame not to pay attention. What it does in health is going to impact patients, populations, and all levels of healthcare for every country. The retreat of U.S. donors and global health development funding means China is positioning itself as a practical partner for Africa, for Southeast Asia, for Latin America and it’s offering its own model that we’ve discussed, at an incredible pace.
It’s not naive to think about the fact that we should be trying to understand each other better. Geopolitics does get in the way, but also there is so much opportunity. For me, always coming from the clinical and scientific standpoint, understanding China better builds more opportunity to absorb the best of what it is offering.

Robert Postings is a freelance journalist in London, previously based in China and Jordan. He has written for The Times, Time Out Shanghai, China Minutes, The Defense Post, and more. He is a co-founder of the China Correspondents Club of London, New Tide Media Network, and is a director of the editorial leadership team at Young China Watchers. You can find him on LinkedIn.




